Inside This section
Arthroscopic Acromioplasty
Impingement Syndrome
This condition occurs when the Supraspinatus tendon rubs on the under surface of an extension of the shoulder blade known as the Acromium. This results in a painful shoulder which is exacerbated with lifting the arm to or above shoulder height and is usually painful to sleep on at night.
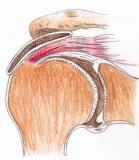
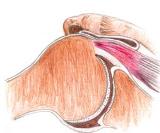
This condition can come on gradually or acutely. The initial injury which may be traumatic or overuse in nature, results in inflammation and swelling in the supraspintus tendon leading to a decrease in the relative space for it under the acromium, as it continues to catch the inflammation and pain worsens, this leads to inhibition of the other muscles in the rotator cuff. One of their roles is to counteract the pull of the deltoid muscle, as they are inhibited and weaken; the deltoid pulls the humeral head upwards further narrowing the subacromial space leading to increasing impingement.
To view an animation of shoulder impingement see the video below
To view a video of Arthroscopic Acromioplasty, click here.
Normal shoulder movement occurs both at the shoulder joint and the shoulder blade rotating on the back. Because with impingement normal movement at the shoulder joint becomes painful, patients compensate by increasing the amount of movement at the shoulder blade this results in 2 problems, firstly the muscles responsible for elevation of the scapula get overloaded and spasm leading to pain around the top of the shoulder blade and up into the neck. Secondly these muscles drag the shoulder blade over the shoulder joint further narrowing the subacromial space.
The presence of a subacromial spur will also decrease the subacromial space. This spur develops over time on the undersurface of the acromium and is very common. It should be noted that the spur itself does not cause the impingement syndrome as it will almost always have been present before onset of symptoms, but in a small number of people it may prevent recovery with non operative treatment.
The mode of treatment therefore is:
- Decrease inflammation with anti-inflammatory medications and or subacromial injections of corticosteroids (e.g. cortisone)
- Rehabilitate the rotator cuff and scapula musculature with a theraband strengthening programme.
- Correct scapula posture with postural retraining and stretches
Adherance to these principles will lead to full recovery in 3- 4 months in around 80% of patients
The strengthening, postural retraining and stretching components are the most important and should be performed at least twice a day.
If the shoulder fails to improve an MRI should be considered to assess other joint pathology such as a rotator cuff tear (ultra sound scans are unreliable)
If the shoulder has not recovered with appropriate non operative management, the next step to consider is surgery, with the treatment of choice being an arthroscopic subacromial decompression. This is keyhole surgery, usually performed under a combination of general anaesthetic and a nerve block, it may be performed as a day stay procedure but usually patients are more comfortable if the stay over night.
The operation is performed through 2 small 1 cm incisions. Firstly an arthroscope is inserted into the shoulder from the back and the joint is evaluated for any other problems which may be causing symptoms. The arthroscope is then placed into the subacromial space above the supraspinatus tendon. The subacromial spur is identified and a second incision is made on the outside of the shoulder. A diathermy probe is used to remove soft tissue from spur which is then removed using a high speed burr. The incisions are then sutured and the arm placed in a sling.
Gentle range of motion exercises are started the next day, and the sling is just for comfort and patients are advised to stop using it as soon as possible, sutures are removed at one week post surgery and the theraband strengthening is commenced.
It takes at least 3 months for the shoulder to return to normal post surgery.
